Hey amazing mamas! Let’s be real for a second – breastfeeding is incredible, beautiful, and… sometimes, a little bit ouchy! We’re talking about those moments when something just doesn’t feel right with your breasts as you navigate this incredible breastfeeding journey. One of those “uh-oh” moments can be breastfeeding with mastitis.

Now, don’t panic! Hearing the word “mastitis” can sound scary, but knowledge is power, right? As your friendly neighborhood breastfeeding specialist and nurse, I’m here to break it down in a way that’s easy to understand, relatable, and maybe even a little bit fun. Because even when things get a little bumpy (pun intended!), we can get through this together!
So, grab a comfy seat (maybe with an ice pack nearby if you’re already feeling the boob blues!), and let’s dive into the world of breastfeeding with mastitis. We’ll cover what it is, what it feels like, and most importantly, what you can DO about it to get back to enjoying those precious breastfeeding moments with your baby.
What in the World is Mastitis Anyway?
Let’s start with the basics. According to the awesome folks over at the Cleveland Clinic, mastitis is basically breast inflammation that can sometimes turn into an infection. Think of it like this: your breast is having a bit of a party, but not the fun kind! It’s more like a “something’s not quite right” kind of party, and sometimes, uninvited guests (bacteria) can crash the party and make things even more uncomfortable.
In simple terms, mastitis is painful inflammation in your breast tissue that can lead to a bacterial infection. Anyone can technically get mastitis, but it’s way more common in us breastfeeding mamas. While it’s rare, even men and women who don’t breastfeed can get it. But for us mothers out there providing liquid gold for our little ones, it’s something we should be aware of.
And how common is it? Well, you are definitely not alone if you experience mastitis. It affects up to 10% of women in the US and maybe even up to 30% of breastfeeding women globally! It’s most common in the first three months after your baby arrives, when you’re still figuring out the breastfeeding dance and your milk supply is establishing itself.
Uh Oh, What Are the Symptoms of Mastitis?
Okay, so how do you know if you might be dealing with mastitis? Think “inflammation,” remember? That means things are going to be swollen, tender, and maybe even a little warm to the touch. Your breasts might feel super full (engorged), but not in a good, “milk-machine-working-perfectly” way.

Here are some symptoms of mastitis that you might experience:
- Breast pain (mastalgia) or a burning sensation: And this isn’t just a little soreness! This pain can really ramp up, especially when your baby is nursing.
- Hard lumps in your breast: You might feel knots or firm areas that weren’t there before.
- Red marks on your breast: Think streaks of redness, warmth, or just an angry-looking patch on your breast.
- Flu-like symptoms: Yep, just when you thought you were over the postpartum exhaustion, mastitis can throw in fever, chills, aches, and that generally yucky feeling.
Engorgement itself is super common, especially in those early days when your milk is coming in – usually in the first few days after giving birth. But engorgement can stick around as long as you’re making breast milk. Mastitis can sometimes feel like engorgement on steroids!
So, What Causes This Booby Blunder?
Let’s get down to the nitty-gritty – what actually causes mastitis? The most common culprit is hyperlactation, or an oversupply of milk. Whoa, wait, too much milk can be a bad thing? Sometimes! When you have an oversupply, it can cause your milk ducts to get a little squeezed. Imagine trying to get too much juice through a straw – things get backed up! The surrounding tissue puts pressure on the ducts, leading to engorgement. This type of mastitis is known as inflammatory mastitis.

Now, here’s where things can get a bit trickier. Inflammatory mastitis can sometimes turn into bacterial mastitis. This happens when bacteria sneak in – often from your baby’s mouth or your skin – and cause an infection due to the inflammation.
And sometimes, in rare cases, abacterial infection can lead to an abscess. Think of an abscess as a collection of fluid (like pus) that needs to be drained by a healthcare provider. We definitely want to avoid that!
Risk factors for mastitis? Well, if you are breastfeeding and have an oversupply of milk, you are at a slightly higher risk.
Now, listen up, because this is important information! For a long time, the advice was to empty your breasts more often if you had an oversupply. But guess what? Research has shown that actually makes engorgement WORSE! Yup, emptying your breast more than usual (think extra pumping or feeds) actually signals your body to make more milk, which can just aggravate the inflammation even more. Crazy, right?
Doc, Am I Sure It’s Mastitis? How Is It Diagnosed?
Wondering how your doctor or healthcare provider figures out if it’s mastitis? Well, they are pretty awesome detectives! Usually, a physical exam and talking about your symptoms is enough for them to make a diagnosis. They will check out your breasts, ask about your pain, fever, and all those lovely symptoms.
If you aren’t breastfeeding and experiencing these issues, your provider might suggest a mammogram or breast ultrasound just to rule out other breast conditions, like (and this is rare, but they need to check) breast cancer.
Okay, Okay, How Do We Treat This Thing?
Alright, let’s talk treatment! The goal with mastitis treatment is to dial down the inflammation, ease the pain, and prevent an infection from setting up shop (or if it’s already there, to kick it to the curb!). Remember, researchers are always learning more about lactation and mastitis, so always chat with your healthcare provider to make sure you are getting the most up-to-date information and care.
Now, get this – the old school advice for mastitis treatment used to be heat, massage, and extra pumping or breastfeeding. But guess what? Times have changed! Many providers now recommend treating inflammatory mastitis more like a sprained ankle. Think about it – would you massage a swollen, sprained ankle or put a heating pad on it? Nope! You’d reach for the ice! It’s the same idea with mastitis. The swelling is mostly from the tissues around the milk ducts, not some “milk plug” that needs to be “worked out.” We need to reduce the inflammation to help the milk flow better.
So, what can you do at home to treat inflammatory mastitis? Think RICE – Rest, Ice, Compression… well, sort of!
- Ice, Ice, Baby!: Forget the heat! Grab an ice pack or a bag of frozen veggies (peas work great!). Apply it to your breast to reduce swelling. Pro tip: lie on your back while icing so the swelling can drain into your lymph nodes.
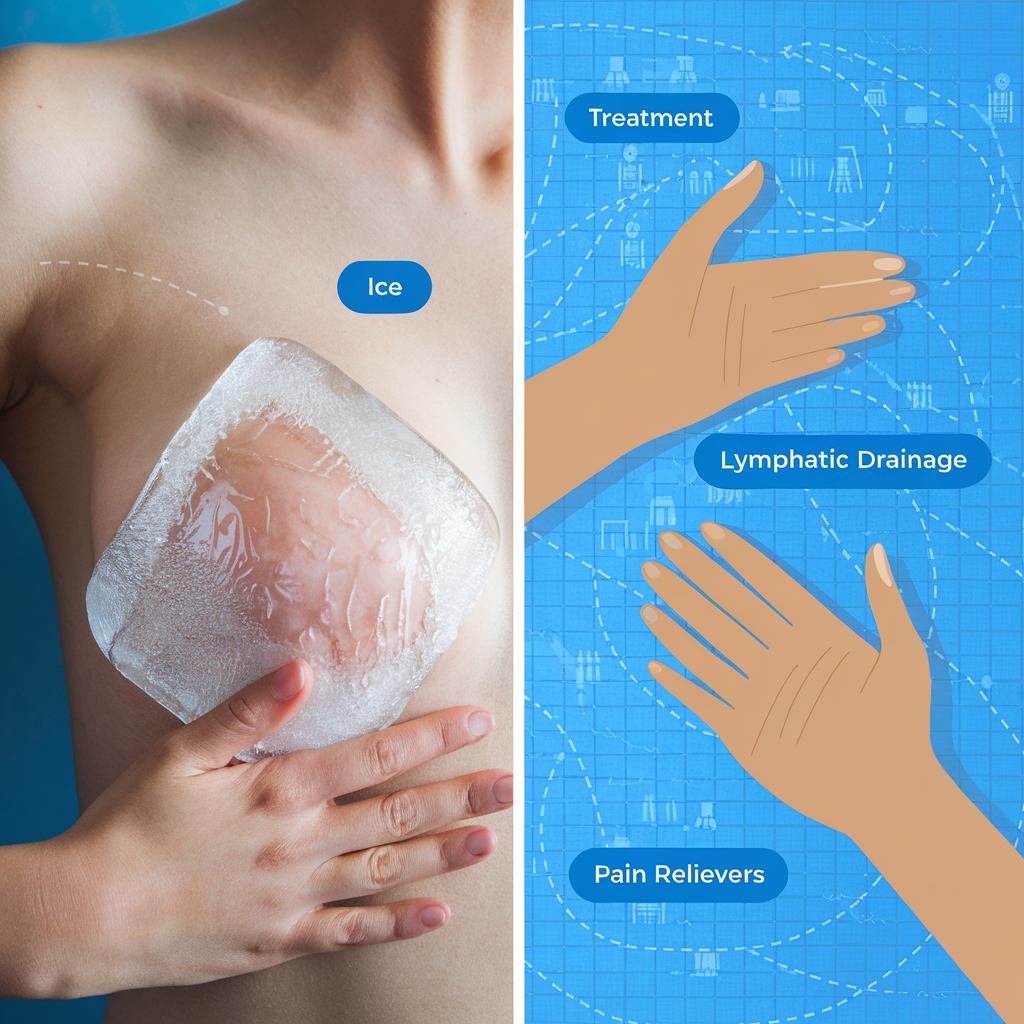
- Pain Relievers: Over-the-counter NSAIDs (nonsteroidal anti-inflammatory drugs) like ibuprofen (Advil, Motrin) or naproxen (Aleve) are your friends! They help reduce both swelling and pain. Always check with your doctor to make sure these are safe for you, especially postpartum.
- Lymphatic Drainage: This is like a super gentle “petting a cat” massage. Using very light pressure, stroke your breast towards your lymph nodes – these are located above your collarbones and in your armpit. This gentle motion helps move fluid and reduce swelling. We’re talking light touch here, not deep tissue massage!
- Reverse Pressure Softening (RPS): This fancy-sounding technique is actually pretty simple and can be a lifesaver, especially if your areola and nipple are super swollen and making it hard for baby to latch. To do RPS, place two fingertips around the base of your nipple. Apply gentle pressure, then slowly drag your fingers away from your nipple. Do this at different angles all around your nipple. This helps move fluid away from the nipple area and can make latching easier.
- Wear a Supportive Bra: A good, supportive bra can make a difference, but make sure it’s not too tight! You want support, not extra pressure on your already tender breasts.
Things to Avoid When You Have Mastitis

- Aggressively massage your breast: Remember, gentle lymphatic drainage is okay, but no deep tissue massage!
- Massaging devices: Put those away for now!
- Soaking your breast: No baths, no compresses, no soaking!
- Heat: Just say no to heat! Ice is your friend.
When Antibiotics Might Be Needed
If those at-home treatment methods for inflammatory mastitis aren’t helping after a day or two, or if things seem to be getting worse, it might be bacterial mastitis. In this case, your healthcare provider will likely prescribe antibiotics to clear up the bacterial infection in your milk ducts.
These antibiotics usually work pretty quickly, and you should start feeling better within 48 to 72 hours. Keep taking the full course of antibiotics, even if you feel better! Over-the-counter pain relievers can still help with discomfort, but they won’t fight the infection itself.
Complications? Eeek!
What happens if mastitis is left untreated? Well, sometimes a breast infection like mastitis can lead to a breast abscess.
Like we talked about, this is a collection of pus that usually needs to be drained by a healthcare provider, sometimes even surgically. That’s why it’s so important to seek care and treatment early!
How Long Does This Mastitis Misery Last?
Good news! Inflammatory mastitis usually gets completely better within 10 to 14 days, especially with the right care.
You should start seeing a big improvement in your symptoms within 24 to 72 hours of starting treatment. Recognizing those early signs of engorgement and inflammation is key because then you can jump on the treatment methods quickly and get relief sooner!
Can I Still Breastfeed with Mastitis? PLEASE Say Yes!

YES! Absolutely, YES! It is not only safe but actually recommended to keep breastfeeding when you have mastitis. Your baby cannot get a breast infection from your breast milk. In fact, breast milk is packed with amazing antibacterial properties that actually help babies fight off infections! How cool is that? And the antibiotics your provider prescribes for mastitis are usually totally safe for your baby.
It might be uncomfortable to nurse with mastitis, but keep going! Frequent milk removal is important. Think of it as treatment too!
Can This Happen Again? Mastitis Part Two?
Unfortunately, yes, mastitis can sometimes come back. Some mothers experience it more than once.

Prevention is Key: Let’s Keep Mastitis Away!
So, how can we try to prevent mastitis in the first place? Here are some tips:
| Pump Smart, Not Hard: | A great rule of thumb is to only pump what your baby actually needs. If you’re breastfeeding directly, don’t feel like you need to pump afterwards to “empty” your breast completely. Over-pumping can signal your body to make even more milk, which, as we know, can contribute to mastitis. |
| Latch Like a Pro: | Talking to a lactation consultant or attending a breastfeeding class can be incredibly helpful to learn what a good latch looks and feels like. A good latch helps your baby efficiently remove milk, and it also helps your body naturally adjust milk production to your baby’s needs. |
| Bra Bliss: | Ditch the super tight bras!Don’t wear tight-fitting bras. They can restrict milk flow and increase your risk of mastitis. |
| Skip the Nipple Shells: | Avoid using nipple shells or other devices on your breasts unless specifically recommended by your healthcare provider or lactation consultant. These can sometimes put pressure on milk ducts. |
The Outlook is Bright!

Mastitis is definitely a pain (literally!), and it’s super uncomfortable, but it usually doesn’t cause any long-term health problems. With at-home treatment and maybe antibiotics if needed, most mothers recover completely and continue their breastfeeding journey.
You might notice you make a little less milk temporarily while your body is fighting off the inflammation or infection, but your milk supply should bounce back as you start feeling better.
And just to put your mind at ease – mastitis does not increase your risk of breast cancer. However, some symptoms of mastitis can be similar to a rare type of breast cancer called inflammatory breast cancer. This type of cancer causes changes in the breast skin, like dimpling or a rash that looks like orange peel skin. Like mastitis, it can also cause redness and swelling. But inflammatory breast cancer usually doesn’t cause breast lumps. Inflammatory breast cancer is aggressive and needs prompt diagnosis and treatment. So, the bottom line? Any time you notice new breast changes, always check in with your healthcare provider right away, just to be safe!
When to Call Your Healthcare Provider – Don’t Wait!

When should you reach out to your healthcare provider? Don’t hesitate to call if:
- At-home treatment for engorgement isn’t helping, and you suspect mastitis.
- You have breast pain.
- You notice changes in how your breasts feel.
- You find a new lump in your breast.
- You have nipple discharge (especially if it’s bloody or pus-like).
- Your symptoms are getting worse even after 24 hours of antibiotics or several days of at-home treatment.
Questions to ask your doctor:

Don’t be shy! Ask your doctor:
- Why did I get mastitis?
- How long will it last?
- What’s the best treatment for me?
- What can I do to prevent mastitis from coming back?
- Are there any signs of complications I should watch out for?
ER or Doctor’s Office?
Usually, you can see your regular doctor or healthcare provider for mastitis. Going to the ER is rarely needed. However, if your symptoms are rapidly worsening, you have a very high fever, or you’re really concerned and can’t get in to see your provider quickly, then going to the ER might give you peace of mind. If you’re already on antibiotics and your fever and swelling are getting worse, they might want to do some imaging to rule out an abscess.
Mastitis or Just a Clogged Duct? What’s the Difference?

Sometimes, it can be tricky to tell the difference between mastitis and a clogged milk duct (sometimes called “plugged” duct). “Clogged ducts” are basically areas of inflammation or engorgement around the ducts that make it harder for milk to flow. If inflammation from a “clogged duct” isn’t treated, it can lead to mastitis.
Think of a clogged duct as a little traffic jam in your milk highway. Mastitis is like the whole highway is under construction and everything is backed up and inflamed!
Read more: Overcoming Breastfeeding Challenges: Tips from a Breastfeeding Specialist
You’ve Got This, Mama!

Any breast change can be a little unnerving, and mastitis is definitely no fun. But remember, you are not alone! So many breastfeeding mothers experience mastitis. The key is to recognize the symptoms early and get the right care and support. If you develop mastitis while breastfeeding, reaching out to a lactation consultant can be a game-changer. They can help ensure you and baby have a good latch and give you personalized breastfeeding tips to help prevent future issues.
Breastfeeding is an amazing journey, but it’s okay if there are bumps along the road. Take care of yourself, listen to your body, and don’t hesitate to ask for help from your healthcare provider or a lactation professional. You are a super mama, and you’ve got this!
Frequently Asked Questions:
Can you continue breastfeeding with mastitis?
Yes, it’s safe to continue breastfeeding with mastitis. In fact, nursing can help clear the infection by keeping milk flowing. Suddenly weaning may worsen your symptoms. If you need support, a lactation consultant can provide guidance and relief strategies.
Can babies drink milk with mastitis?
Yes, your milk is still safe for your baby to drink, even if you have mastitis. While you may feel unwell, mastitis does not harm your breast milk or your baby.
How to stop breastfeeding with mastitis?
If you need to stop breastfeeding while dealing with mastitis, wean gradually by slowly reducing feedings rather than stopping abruptly, as sudden weaning can worsen inflammation and discomfort. A lactation consultant or doctor can help you navigate the process safely.
Can I keep breastfeeding with mastitis?
Yes, you should continue breastfeeding with mastitis. Frequent nursing helps drain blocked ducts and clear the infection. Your milk is still safe for your baby, though it may have a slightly salty taste due to the infection.
How to wean off breastfeeding with mastitis?
If you need to wean while dealing with mastitis, do so gradually by dropping one feeding at a time to prevent engorgement and worsening symptoms. Consulting a doctor or lactation consultant can help you manage mastitis while weaning safely.
Find Practical Mom Tips to Make Life Easier!

Breastfeeding is a journey, and I’m here to support you every step of the way. If you’re looking for even more practical advice, real-life tips, and encouragement, be sure to check out my YouTube channel!
Whether you’re tackling common breastfeeding challenges or just need a confidence boost, you’ll find a wealth of resources to help you thrive on this amazing journey. Click here.







