Are you dreaming of those sweet, cozy moments breastfeeding your little one? It’s truly a special experience, a beautiful dance between you and your baby. But sometimes, this dance feels more like a clumsy tango tripping over unexpected hurdles! If you’re expecting, already in the thick of breastfeeding, or caring for a little one, you’ve come to the right place. I’ve chatted with countless women, just like you, about the ups and downs of breastfeeding. And guess what? You are SO not alone and let’s start overcoming breastfeeding challenges!

In this blog, I’ll equip you with the knowledge and support you need to feel confident and empowered on your breastfeeding journey. Ready to get started? Let’s jump in!
What are Breastfeeding Challenges Anyway?
So, what exactly are these “breastfeeding challenges” we keep talking about? Well, simply put, there are any bumps in the road that make breastfeeding feel harder than it should be. And trust me, there’s a whole spectrum! From minor nipple pain that makes you wince to feeling like your milk supply is playing hide-and-seek, to dealing with uncomfortable breast engorgement – it’s all part of the breastfeeding adventure for many moms.

It’s super important to know that experiencing breastfeeding challenges doesn’t mean you’re doing anything wrong. It just means you’re a normal woman navigating a natural process that sometimes needs a little support and understanding. Think of learning to ride a bike – you might wobble, and fall a few times, but eventually, with practice and maybe some helpful tips, you’ll be cruising! Breastfeeding is similar. It’s a learning process for both you and your baby.
Common Breastfeeding Challenges: Let’s Talk Real
Alright, let’s get down to brass tacks and talk about some of the common breastfeeding challenges women face. Knowing what’s normal and what steps to take is half the battle!
Ouch! Sore Nipples
Sore nipples are like the uninvited party guest of early breastfeeding – they show up when you least expect them and can really put a damper on things. But guess what? Nipple pain, especially in the first week or so, is actually quite common. Think of it as your nipples getting used to their new job!
What causes sore nipples?
Usually, sore nipples are a signal that your baby isn’t latching on to your breast deeply enough. Imagine your nipple being pinched or pulled instead of comfortably drawn into your baby‘s mouth. Ouch, right? Other culprits can include:
- Incorrect latch: This is the BIG one. If the baby is only sucking on the nipple and not taking a good portion of the areola (the darker area around your nipple) into their mouth, it can lead to friction and soreness.
- Improper positioning: Sometimes, the way you’re holding your baby can contribute to a shallow latch.
- Thrush: This yeast infection can affect both the baby‘s mouth and your nipples, causing nipple pain.
- Pumping issues: Using a breast pump with flanges that are the wrong size or using too high suction can also lead to sore nipples.
Tips to Soothe Sore Nipples and Get Relief:
| Perfect the Latch: | This is KEY! Work with a lactation consultant or nursing staff to ensure your baby has a deep, comfortable latch. Think “nose to nipple” and bring baby to your breast, not the other way around. Baby‘s mouth should be wide open, like a big yawn, and their lips should be flanged out like fish lips. You can learn more about proper latching techniques from support groups and lactation professionals. |
| Check positioning: | Experiment with different breastfeeding positions (cradle hold, cross-cradle, football hold, laid-back breastfeeding) to find what’s most comfortable for both you and baby. |
| Air dry nipples: | After breastfeeding, let your nipples air dry completely. Milk and air are natural healers! |
| Apply breast milk: | Your own breast milk is liquid gold! Express a few drops and gently rub it on your nipples after each feed. It has natural healing properties. |
| Use a nipple cream: | Lanolin creams can provide soothing relief. Apply a thin layer after breastfeeding. |
| Breast pads: | Choose breast pads that are breathable and change them frequently to keep your nipples dry and prevent infection. |
| Consider nipple shields (temporarily): | If pain is severe, nipple shields can offer temporary relief while you work on improving the latch. However, use them under the guidance of a lactation consultant, as prolonged use can sometimes affect milk supply. |
| Rule out thrush: | If nipple pain is sudden, burning, and doesn’t improve with latch correction, consider thrush. See your doctor or baby‘s pediatrician for diagnosis and treatment. |
| Warm compress: | A warm compress before breastfeeding can help with milk flow and make latching more comfortable. |
Remember, nipple pain should improve significantly within the first week or two. If the pain is severe, persistent, or worsening, please call your doctor or lactation consultant for help. Don’t suffer in silence – support is available!
Engorgement: When Breasts Feel Like Rocks
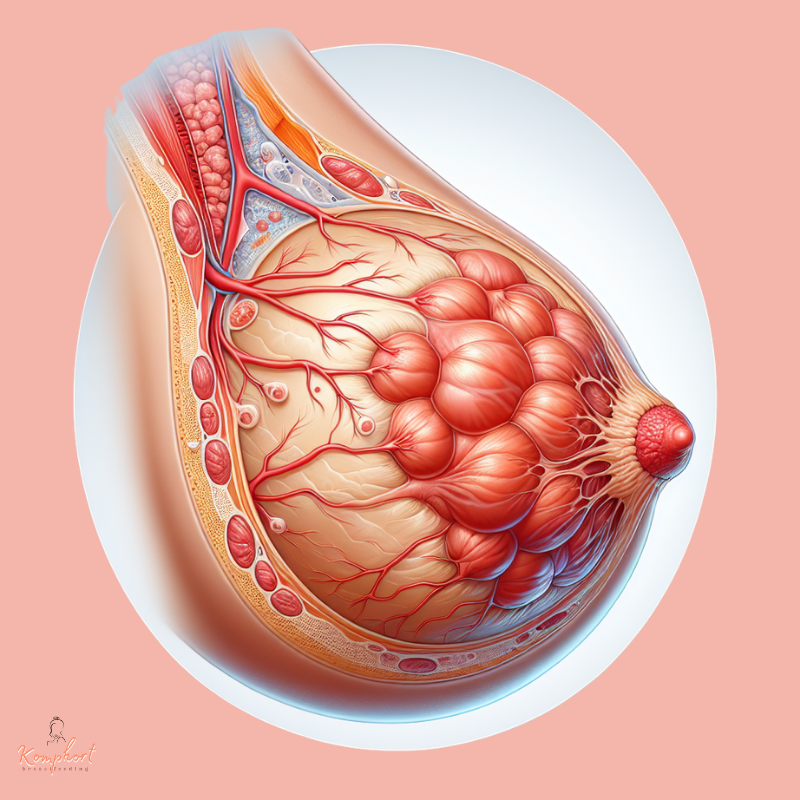
Breast engorgement is when your breasts become overly full of milk. Think of it as your milk coming in with full force! This usually happens a few days after the baby is born when your milk supply is transitioning from colostrum to mature milk. While it’s a sign that your milk is indeed “in,” engorgement can be quite uncomfortable, making your breasts feel hard, swollen, and sometimes even painful.
Why does engorgement happen?
- Increased blood flow and milk production: After birth, hormonal changes signal your body to ramp up milk production. Increased blood flow to the breasts also contributes to swelling.
- Infrequent or ineffective milk removal: If the baby isn’t breastfeeding frequently enough or latching effectively to remove milk, it can build up and cause engorgement.
Tips to Relieve Engorgement:
| Frequent breastfeeding: | Nurse your baby frequently, at least 8-12 times in 24 hours, and on demand. This is the best way to relieve engorgement. |
| Effective latch: | Ensure the baby has a good, deep latch to efficiently remove milk. |
| Warm compress or shower: | Applying a warm compress or taking a warm shower before breastfeeding can help stimulate milk flow and soften the breast, making latching easier for the baby. |
| Hand expression or pumping: | If your breasts are too full and hard for the baby to latch comfortably, express a little milk by hand or with a pump to soften the areola before offering the breast. Pump or express only enough to soften the breast, not to empty it completely, as excessive pumping can signal your body to produce even more milk, potentially worsening engorgement. |
| Cold compress: | After breastfeeding, apply a cold compress or chilled cabbage leaves (yes, really!) to your breasts for 15-20 minutes to reduce swelling and pain. |
| Reverse pressure softening: | If your areola is very firm due to engorgement, reverse pressure softening can help. Gently press your fingertips around the base of your nipple for a few minutes to push some fluid back and soften the areola, making latching easier. |
| Pain relievers: | Over-the-counter pain relievers like ibuprofen or acetaminophen can help manage pain and discomfort. |
Engorgement is usually temporary and resolves within a few days as your milk supply adjusts to your baby‘s needs. However, if engorgement is severe, painful, or accompanied by fever or other signs of infection, call your doctor.
Plugged Milk Ducts: Ouch, That Knot!

A plugged milk duct feels like a tender lump or knot in your breast. It happens when a milk duct gets blocked, causing milk to back up. It can be painful and sometimes lead to mastitis if not addressed.
What causes plugged ducts?
- Infrequent or ineffective milk removal: Just like with engorgement, if milk isn’t removed effectively, it can become thick and plug a duct.
- Pressure on the breast: Tight bras, underwire bras, or even sleeping in a position that puts pressure on your breast can contribute to plugged ducts.
- Dehydration and fatigue: Not drinking enough fluids or being overly tired can also play a role.
- Sudden change in breastfeeding routine: Going too long between feeds or skipping feeds can sometimes trigger a plugged duct.
Tips to Clear a Plugged Duct:
| Frequent breastfeeding: | Keep breastfeeding frequently! Start feeds on the affected side. Your baby‘s suckling is the most effective way to clear a plugged duct. |
| Warm compress and massage: | Apply a warm compress to the affected area for 5-10 minutes before breastfeeding. Gently massage the lump while the baby is nursing, moving towards the nipple. You can also massage in a warm shower. |
| Vary breastfeeding positions: | Try different breastfeeding positions to help drain all areas of your breast. Positions where the baby‘s chin points towards the plugged duct can be particularly helpful. |
| Hand expression or pumping: | After breastfeeding, try hand expression or pumping to further drain the breast. |
| Rest and hydration: | Get plenty of rest and drink lots of fluids. |
| Loose clothing: | Avoid tight bras or clothing that puts pressure on your breasts. |
| Learn about lecithin: | Some women find that taking lecithin, a natural food supplement, helps to reduce the recurrence of plugged ducts by making milk less sticky. Talk to your doctor or lactation consultant before starting any supplements. |
Most plugged ducts resolve within a day or two with these self-care measures. However, if you develop fever, flu-like symptoms, or the redness, pain, and warmth in your breast worsen, it could be mastitis, and you should call your doctor promptly.
Mastitis: Breast Infection – Know the Signs
Mastitis is a breast infection that can develop when a plugged milk duct isn’t cleared, or bacteria enter the breast through a cracked nipple. It’s important to recognize mastitis early so you can get treatment and feel better quickly.
Symptoms of mastitis:
- Breast pain or tenderness
- Warmth, redness, and swelling in a wedge-shaped area of the breast
- Fever (101°F or higher)
- Flu-like symptoms: chills, body aches, fatigue
- Sometimes a plugged duct is also present
What to Do If You Suspect Mastitis:
| Call your doctor: | Mastitis usually requires antibiotics to treat the infection. Don’t delay seeking medical help. |
| Continue breastfeeding: | It’s safe and important to continue breastfeeding even with mastitis. Frequent milk removal helps to clear the infection and prevent abscess formation. |
| Rest and fluids: | Get plenty of rest and drink lots of fluids to support your body’s healing process. |
| Warm compress and massage: | Apply warm compresses to the affected area and gently massage while breastfeeding or pumping. |
| Pain relievers: | Over-the-counter pain relievers can help manage pain and fever. |
| Follow the doctor’s instructions: | Take antibiotics as prescribed and complete the full course, even if you start feeling better. |
Mastitis can feel pretty miserable, but with prompt medical care and self-care, you’ll be back on your feet and breastfeeding comfortably soon. If you’re concerned about infection, always call your medical provider.
Low Milk Supply: Is Baby Getting Enough Milk?
Worrying about low milk supply is a very common concern for breastfeeding moms. It’s natural to wonder if your baby is getting enough milk. But before you panic, let’s understand what low milk supply really means and how to address it.
Signs that baby is getting enough milk:

- Weight gain: Baby is gaining weight steadily after the initial newborn weight loss (check with pediatrician for expected weight gain).
- Diaper output: Baby has enough wet and dirty diapers (typically 6 or more wet diapers and 3-4 stools per day after the first few days).
- Satisfied after feeds: Baby seems content and satisfied after breastfeeding sessions.
- Breast softening after feeds: Your breasts feel softer after the baby has breastfed.
- Hearing baby swallow: You can hear or see baby swallowing during feeds.
Possible Signs of Low Milk Supply (and What to Do):
| Poor weight gain: | Baby is not gaining weight adequately. Call your pediatrician. |
| Decreased diaper output: | Fewer than 6 wet diapers in 24 hours after the first few days. Call your pediatrician. |
| Baby seems constantly hungry and fussy: | While some fussiness is normal if the baby is persistently fussy and shows hunger cues soon after feeds, it might be a concern. Observe feeding cues and call a lactation consultant. |
| Breasts don’t feel softer after feeds: | This can be a less reliable indicator after the milk supply is well established. |
Tips to Boost Milk Supply (if needed, after consulting with a professional):
| Frequent and effective milk removal: | Nurse baby frequently and on-demand, at least 8-12 times in 24 hours. Ensure a good latch so the baby can effectively remove milk. |
| Offer both breasts: | Offer both breasts at each feeding. |
| Pump after feeds (if needed): | If the baby isn’t effectively draining the breast or you need to increase milk supply, pump for 10-15 minutes after breastfeeding sessions. |
| Power pumping: | This technique involves pumping frequently for short durations to mimic cluster feeding and signal your body to produce more milk. Learn more about power pumping from lactation resources. |
| Skin-to-skin contact: | Spend time holding your baby skin-to-skin. This releases hormones that promote milk production. |
| Ensure adequate calorie intake and hydration: | Eat a balanced diet and drink plenty of fluids. While milk-boosting foods and drinks (like oatmeal, fenugreek, and lactation cookies) are often discussed, focus on overall nutrition and hydration first. Read: Best Lactation Cookies: Your Guide to Delicious Milk-Boosting Recipes |
| Rest: | Get as much rest as possible. Fatigue can impact the milk supply. |
| Rule out medical causes: | In rare cases, medical conditions can contribute to a low milk supply. Discuss concerns with your doctor and baby‘s pediatrician to rule out any underlying problems. |
| Medications or herbal galactagogues (under professional guidance): | In some situations, medications or herbal supplements called galactagogues might be considered to boost milk supply, but always discuss these options with your doctor or lactation consultant. These are generally not the first line of action and should be used under medical supervision. |
It’s crucial to assess milk supply concerns with the help of a lactation consultant or your pediatrician. They can evaluate the baby‘s weight gain, feeding patterns, and diaper output to determine if there’s truly a low milk supply issue and help create a plan to address it.
Getting Support: You Are Not Alone!

Remember, overcoming breastfeeding challenges is definitely doable, and you absolutely don’t have to do it alone! There is a fantastic network of support and resources available to help you thrive on your breastfeeding journey.
Where to find support:
- Lactation Consultants (IBCLC): These are the superheroes of breastfeeding support! They are experts in breastfeeding management and can help with latch issues, milk supply concerns, pain, and any other breastfeeding challenges. Find an IBCLC in your area through organizations like the International Lactation Consultant Association (ILCA).
- La Leche League: This international organization offers peer-to-peer support for breastfeeding moms. They have local groups, meetings, and support groups where you can connect with other breastfeeding women and learn from experienced leaders.
- Hospital and birthing center nursing staff: The nursing staff at your hospital or birthing center are valuable resources in the early days after birth. Don’t hesitate to ask for help and guidance while you are there.
- WIC (Women, Infants, and Children) program: WIC provides breastfeeding support, education, and resources to eligible women. They often have lactation consultants or peer counselors on staff and offer breast pumps in certain situations. Check your local WIC office for eligibility and services.
- Online support groups and forums: Online communities can offer valuable peer support and a place to share experiences and ask questions. However, always be sure to cross-reference any advice with a medical professional or lactation consultant.
- Your pediatrician or family doctor: Your medical providers can also offer guidance and help rule out any medical problems contributing to breastfeeding challenges.
Plan Ahead for a Smoother Start
While you can’t predict every bump in the road, planning ahead can definitely set you up for a smoother breastfeeding start.

Tips to plan ahead:
- Take a breastfeeding class during pregnancy: Educate yourself about breastfeeding basics, latch, positioning, common challenges, and resources. Knowledge is power!
- Pack breastfeeding essentials in your hospital bag: Comfortable nursing bras, nipple cream, breast pads, and a water bottle are good items to have on hand.
- Discuss your breastfeeding plan with your partner and support system: Make sure your support people understand your goals and how they can help you.
- Know where to find support resources: Identify lactation consultants, support groups, and WIC offices in your area before the baby arrives.
Conclusion

Breastfeeding is an amazing gift you give to your baby, and it’s a journey filled with incredible moments of connection. Yes, there might be challenges along the way, but remember – you are strong, capable, and definitely not alone! Overcoming breastfeeding challenges is absolutely possible with the right knowledge, support, and a sprinkle of self-compassion.
So, take a deep breath, learn as you go, reach out for support when you need it, and celebrate every breastfeeding milestone, big or small. You are doing an amazing job, mama! Happy breastfeeding!
Frequently-Asked Questions:
How can I solve my breastfeeding problem?
If you’re struggling with breastfeeding, try adjusting your baby’s latch, nursing frequently, and staying hydrated to support milk supply. For engorgement, use warm compresses before feeding and cold packs after. Clogged ducts can be relieved with massage and nursing on the affected side first. Sore nipples may improve with lanolin and air drying. If let-down is too fast, try laid-back nursing; if too slow, use breast compressions. If challenges continue, a lactation consultant can provide personalized support.
How to deal with breastfeeding failure?
If breastfeeding isn’t going as planned, try offering both breasts at each feed and practicing skin-to-skin contact to boost supply. Seeking help from a lactation consultant, midwife, or health visitor can provide guidance and reassurance. Remember, every feeding journey is unique, and finding what works best for you and your baby is what matters most.
How to persevere with breastfeeding?
To persevere with breastfeeding, stay close to your baby after birth, ensure a good latch, and be patient as you both learn. Feed on demand, keep your baby in the same room, and avoid teats, dummies, or unnecessary supplements to support your milk supply. Seeking support from a lactation consultant can also make a big difference.
Why is breastfeeding challenging?
Breastfeeding can be challenging due to issues like sore nipples, engorgement, mastitis, leaking, pain, and latch difficulties. Without proper support, these problems may lead some mothers to stop breastfeeding earlier than planned. Seeking help from a lactation consultant can make a big difference.
When is the hardest part of breastfeeding?
The first two to three weeks of breastfeeding are often the hardest, as mothers face challenges like soreness, latch issues, and supply concerns. However, those who push through usually find it becomes easier and more rewarding over time.
Find Practical Mom Tips to Make Life Easier!

Breastfeeding is a journey, and I’m here to support you every step of the way. If you’re looking for even more practical advice, real-life tips, and encouragement, be sure to check out my YouTube channel!
Whether you’re tackling common breastfeeding challenges or just need a confidence boost, you’ll find a wealth of resources to help you thrive on this amazing journey. Click here.








